There dermatillomaniaalso known as bruising disorderit is a recurring and difficult to check impulse that leads to teased, scratching or pinching your skin. This behavior, although it may seem like a simple habit, can cause skin lesions, emotional discomfort and have a significant impact on everyday life. In fact, those who suffer from it can spend a lot of time touching the skin or, on the contrary, to fight against the impulse to do it. According to recent studies, this condition affects about 1.4% of the general population, with a significantly greater prevalence in women than men (Farhat et al., 2023).
The areas of the body most commonly affected by this behavior are:
- the face;
- hands;
- the arms;
- the legs.
What is dermatillomania (or bruising disorder)?
To understand thoroughly What is dermatillomaniait is important to go beyond the idea of a “bad habit”. We are talking about compulsive and repetitive behavior, also known as bruising disorder (in English Skin Picking Disorder ), which can lead to considerable discomfort.
The impulse of teasing the skin can manifest itself in two ways: sometimes it is a gesture automaticalmost unaware, which takes place while focusing on something else; Other times it is focusedthat is, a conscious act aimed at removing small skin imperfections perceived.
In both cases, the most affected areas tend to be a face, hands and arms, and the result is a cycle that can leave both physical and emotional signs.
What are the causes of dermatillomania?
The Causes of dermatillomania They are not attributable to a single factor, but to a complex interaction of psychological, neurobiological and environmental elements. Often, at the basis of this behavior there is an attempt, mostly unaware, of regular difficult emotions.
- Psychological factors: The tease of the skin can become a dysfunctional coping mechanism, a strategy for managing intense and overwhelming emotional states like Anxiety, stress, boredom, anger or a deep sense of emptiness. The physical act offers a momentary distraction from inner pain.
- Neurobiological factors: Some research suggests that neurochemical imbalances may be involved, in particular in the brain reward system, which make the behavior difficult to stop once started.
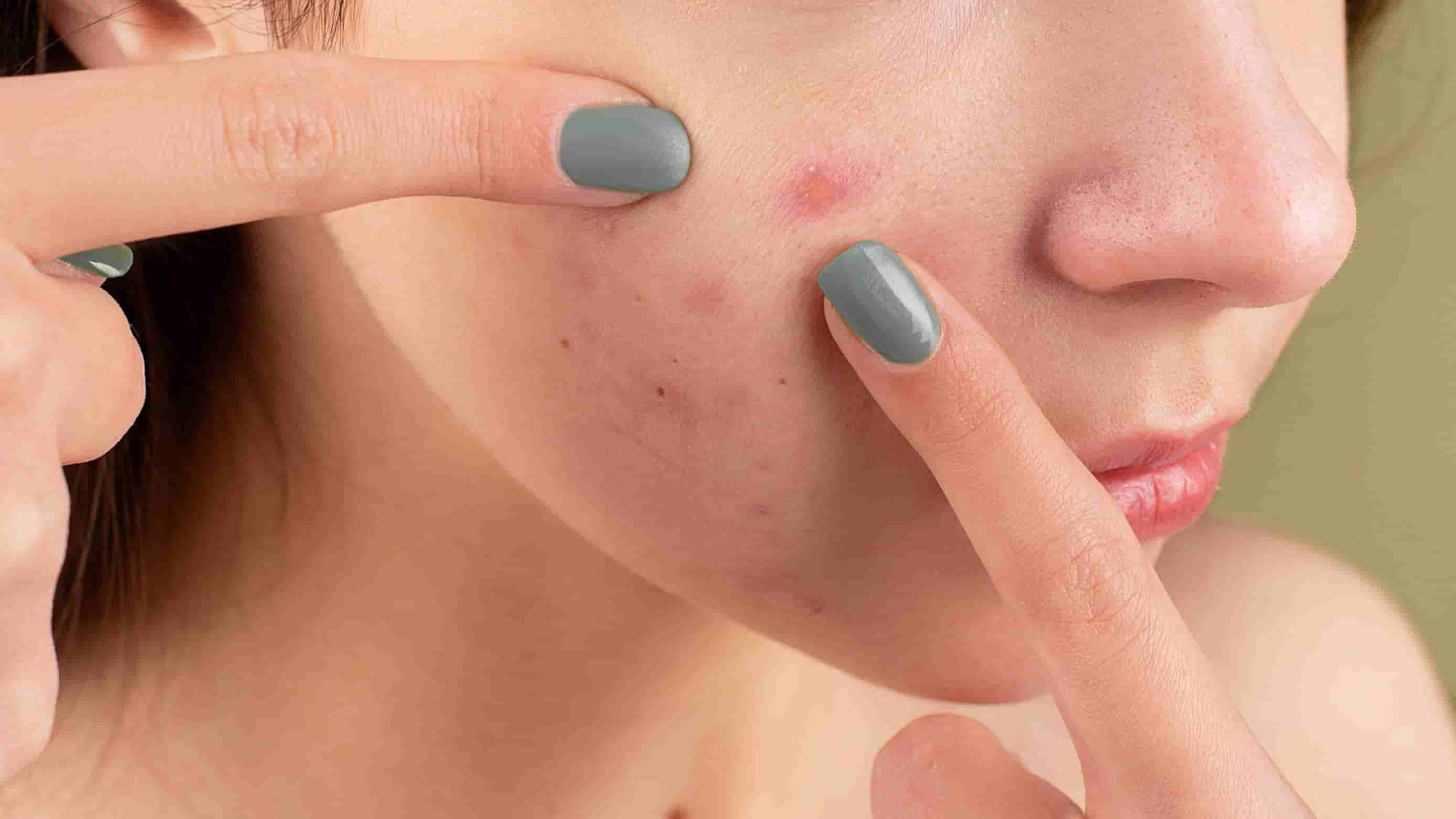
- Triggering factors (trigger): The impulse can be triggered by the vision or tactile perception of small skin imperfections, such as pimples, crusts, calluses or blackheads. The presence of these irregularities can activate the desire to “fix them”, giving way to the compulsive cycle.
How to recognize the disorder
The diagnosis of dermatillomania is formulated by a mental health professional on the basis of specific criteria. In order to speak of bruising disorder, these aspects are generally evaluated:
- The person puts in place recurrent behavior of teased of the skin, that come to cause skin lesions;
- are present repeated attempts to reduce or interrupt This behavior, often without success;
- behavior causes a clinically significant discomfort or a impairment of social, work or other important areas.
Beyond the diagnostic criteria, it is essential to recognize the emotional experience that accompanies this condition. Often, those who suffer from it live a deep sense of impotence And anger In order not to stop, to which they are added sense of guilt And shame For self -inflict injuries.
These emotions can have a negative impact on self -image, leading to hiding the bruises with makeup or clothes and avoid social situations, such as going to the beach, in the gym or in the pool, where the wounds could be visible.
What are the consequences and risks?
Living with bruising disorder can have significant implications that go far beyond the skin (Grant et al., 2012). The consequences occur on several levels, intertwining physical health and psychological well -being.
- Physical consequences: The continuous toothpick can cause skin lesions, bleeding, permanent scars and, in the most serious cases, bacterial infections who can request medical intervention.
- Psychological and social consequences: On an emotional level, the disorder is often accompanied by a heavy load of senses of guilt, shame and embarrassment, who can erode self -esteem. This inner suffering can lead to isolation and toavoidance of social situations (How to attend swimming pools or beaches) for fear of judgment, with a negative impact on interpersonal relationships and working life.
Is it an obsessive compulsive disorder?
This is a very common and important question. In the Diagnostic and statistical manual of mental disorders (DSM-5), the dermatillomania is included in the chapter dedicated to the disorders of the obsessive – compulsive spectrum, But it is classified as a disorder in itself, distinct from the obsessive compulsive disorder (DOC) actual.
The fundamental difference lies in the origin of behavior. In the doc, compulsions (repetitive actions) are a response to intrusive and distressing thoughts (obsessions) and serve to neutralize a fear or prevent damage.
In the dermatillomania, however, repetitive behavior does not arise from an obsession, but has the purpose of alleviate a state of tensionstress or boredom.
While in the DOC concerns can be very varied (fear of contamination, doubts about their relationship, as in the doc doc), in bruising disorder the impulse is focused on the body and on the search for immediate relief from an internal discomfort.
Dermatillomania: how to stop? The care paths
If you are wondering how to stop To tease the skin, it is important to know that there are effective paths (Loftus et al., 2025). Face the dermatillomania It often requires an integrated approach: a dermatological treatment to treat skin lesions and a psychotherapy path to work on the roots of behavior.
Psychotherapy helps to explore the “why” of this impulse: when they manifest, what emotions unleash it and what functions performs. One of the most effective approaches is the cognitive therapy -comphamentamental (TCC)which focuses on the inversion of compulsive habits. The route begins with a phase of car self -employment and collection of information to understand:
- the history and debut of behavior;
- the situations and emotions that trigger it;
- the physical and emotional consequences.
Subsequently, the therapist leads the person in the symptom management, teaching practical strategies. Among these, one of the best known is the Habit Reversal Training (HRT). This protocol helps to increase the awareness of the trigger (thoughts, emotions, situations) and to replace the impulse of teasing the skin with alternative and not harmful behavior.
Other very valid therapeutic approaches, which work on the acceptance of emotions and awareness, include:
- Acceptance and Commitment Therapy (Act);
- there Dialectrical Behavioral Therapy (DBT).
Finding well -being: one step at a time
Face dermatillomania may seem like a solitary and difficult battle, but it is essential to remember that It is not a question of lack of will. It is a complex condition that deserves understanding, empathy and qualified support. Recognizing that you have a problem and looking for information is the first, courageous step towards well -being.
A psychotherapy path can offer you a safe space to explore the emotions that hide behind the impulse of teasing the skin. With the help of a professional, you can develop concrete strategies to manage this behavior and build, one step at a time, a more serene and compassionate relationship with your body and yourself. If you feel that the time has come to take care of you, we are here to support you.

