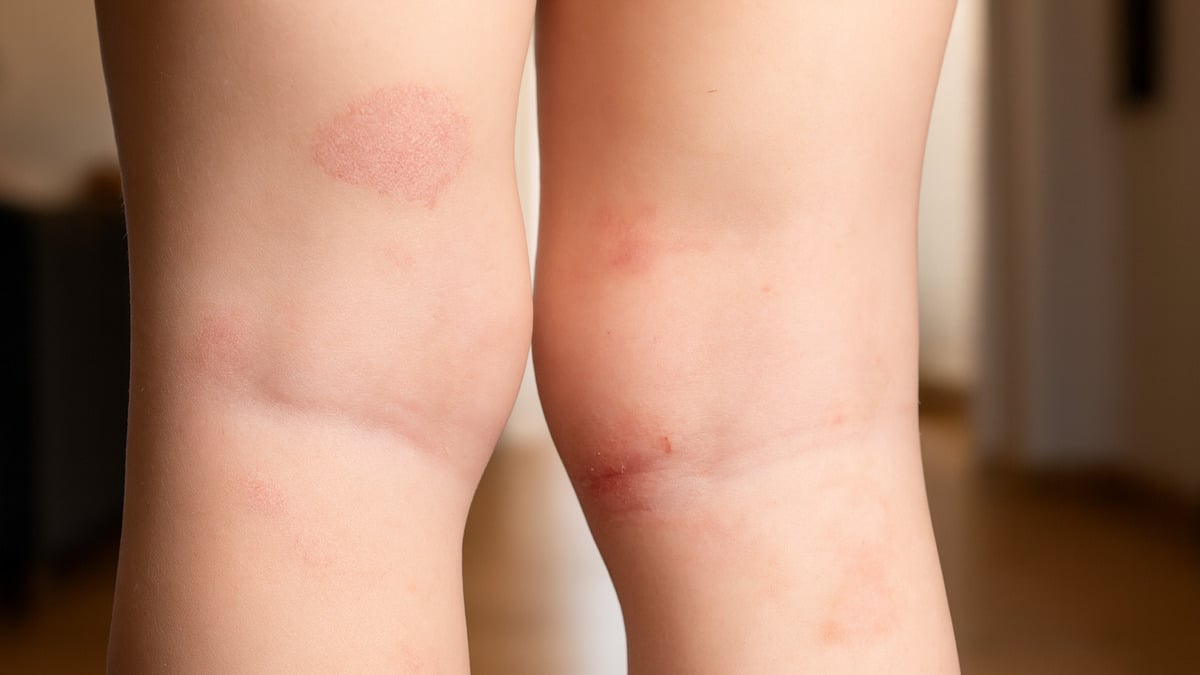
It is a rather widespread infection among children, since being highly contagious, it is easily transmitted in environments where children spend a lot of time together. Let’s find out the causes, symptoms and treatments
Francesca and Michele have just received a communication from the school: a case of ringworm has been reported in their daughter’s class. The term scares them. Is it contagious? How does it manifest itself? Should the child stay at home? And above all: is ringworm in children a serious infection? To answer clearly, it is useful to understand what this infection really is, how to recognize it and how to treat it effectively.
What is ringworm
What is ringworm? It is an infection of the skin, hair or nails caused by dermatophyte fungi, microorganisms that specialize in living where there is keratin, the protein that makes up the most superficial layer of the skin, hair and nails. These fungi are defined as keratinophilic (i.e. “keratin lovers”) and keratinolytic (capable of degrading it to feed on it). This is the reason why ringworm affects the areas rich in keratin and why it tends to cause flaking, hair breakage and superficial lesions.
Ringworm is very common, especially among children. Being a highly contagious infection, it is easily transmitted in environments where children spend a lot of time together – schools, nurseries, gyms – where direct contact or sharing objects favors the passage of the fungus. It is no coincidence that ringworm of the skin or ringworm of the body is one of the most common mycoses in children. The dermatophytes responsible for ringworm are the same ones that are commonly called “skin fungi”.
Ringworm: the causes
Ringworm is caused by three large groups of dermatophyte fungi: Trichophyton, Microsporum and Epidermophyton. These microorganisms have a particular characteristic: they feed on keratin, the protein that makes up skin, hair and nails. It is this specific “appetite” that makes them responsible for the typical skin mycosis.
But not all dermatophytes are the same: they are distinguished based on their “preference” for the host.
- Anthropophilic dermatophytes. They are the ones who prefer humans. They cause infections that tend to be milder, but also more easily transmitted from person to person.
Frequent example in children: Trichophyton tonsurans. - Zoophilic dermatophytes. They come from animals, especially cats, dogs, rabbits and rodents.
They are responsible for often more inflammatory forms, such as microsporic ringworm from Microsporum canis, very common in pediatric age, especially when there is close contact with pets. - Geophilic dermatophytes. They live in the soil and cause rarer infections, usually related to playing or contact with contaminated soil.
This distinction helps to understand how the infection occurred and which fungus is most likely, also guiding therapy.
Symptoms of ringworm
The incubation period of ringworm can vary from a few days to a couple of weeks, after which the typical lesions of the disease appear: rounded or oval spots, with red and slightly raised edges and a lighter centre.
The most common symptom is itching, which can be mild or more intense. In some cases, however, the lesions do not itch at all, which can make the diagnostic suspicion less immediate. The skin in the affected area tends to flake, become dry or red. If ringworm affects the scalp, in addition to flaking, hair breakage at the base may appear, with patches of alopecia.
In the more inflammatory forms – often due to fungi transmitted by animals – the keriona soft and painful swelling, similar to a large “bump” with pus: in this case it is essential to contact the pediatrician quickly.
Where ringworm can appear
Ringworm can affect different parts of the body, and the appearance of the lesions changes somewhat depending on the location. This helps the doctor understand which type it is.
- Tinea corporis. It is the most common form in children. It appears as one or more ring-shaped patches, pink or red, on the arms, trunk, shoulders or neck. They usually itch and tend to spread outwards.
- Tinea capitis. Here the fungus affects the scalp. The hair breaks at the base, leaving patches of alopecia with flaking similar to dandruff.
- Tinea pedis. Rare in young children, more frequent in sporty kids. Causes itching between the toes, flaking skin, small blisters.
- Tinea cruris. It causes a red, itchy rash in the inguinal folds, with well-defined edges. It is favored by sweat and poorly breathable clothing.
- Tinea unguium. Nails become thickened, dull, brittle and may change color.
- Tinea faciei. Ring-shaped lesions on the cheeks or forehead. Sometimes it looks like dermatitis and can be confused with other conditions.
- Tinea barbae, tinea manuum. Much rarer in children, more typical of adolescents or adults.
In general, when ring-like lesions, itching, or persistent scaling are observed on the skin, scalp, or nails, ringworm is one of the first diagnoses to consider.
Ringworm and children
Ringworm is particularly common in children, and this depends on several factors. First of all, their skin is thinner and more delicate, so the spores of dermatophyte fungi can penetrate it more easily. Furthermore, the immune system of the little ones is still maturing, and may not yet be able to effectively fight these microorganisms.
Another reason is linked to community life: at school, nursery, in the gym or in the swimming pool, children share games, spaces, mats, combs, hats. These objects can retain fungal spores, which remain viable for a long time and make contagion much easier.
The most frequent forms in childhood are tinea corporis (the “ringworm of the body”), which presents with the typical ring-shaped spots, and tinea capitis (the “ringworm of the scalp”), more insidious because it can cause temporary alopecia and, if very inflammatory, also complications such as kerion.
How you get ringworm: the ways of contagion
Ringworm is very contagious and can be transmitted in different ways. Contagion occurs mainly through direct contact: skin-to-skin between children or between children and animals (cats, dogs, rabbits are often a source of zoophilic fungi). Indirect contagion is also possible, through contaminated objects such as towels, combs, hats, pillows or shared toys. Fungal spores are very resistant and can remain in the environment for weeks, especially in warm, humid places such as swimming pools, gyms and locker rooms.
Some personal conditions can increase the risk: excessive sweating, small skin wounds, obesity, diabetes or immunosuppression. Contact sports also facilitate transmission.
During pregnancy, ringworm can appear as in any other phase of life: it does not represent a risk for the fetus, but still requires diagnosis and adequate treatment.
When to contact the doctor: the diagnosis
Ringworm often has a characteristic appearance, but for confirmation it is always useful to consult a pediatrician or dermatologist. The diagnosis is based above all on the clinical examination, observing the shape of the lesions and listening to the medical history: where they appeared, if they itch, if there have been other cases at school. When necessary, simple and painless tests are performed:
- a skin scraping, i.e. the removal of small scales from the lesion;
- observation under the microscope with potassium hydroxide (KOH) to see the fungi directly;
- in doubtful or more serious cases, a fungal culture, which allows the exact dermatophyte to be identified.
Cures for ringworm
Ringworm is treatable and, with the correct therapy, heals completely. The duration varies depending on the location of the infection. Below are the main therapeutic strategies:
- Topical antifungals. For mild forms, antifungal creams are used (imidazole, ciclopirox, naftifine, terbinafine), to be applied for 4 weeks.
- Systemic antifungals. When ringworm is extensive, affects the scalp or does not improve with creams, oral medications are needed: griseofulvin, itraconazole, fluconazole or terbinafine.
- Specific shampoos. In tinea capitis, medicated shampoos (e.g. ketoconazole) reduce contagiousness.
Natural remedies, i.e. products such as tea tree oil or neem are not effective. Homeopathic treatments have no evidence.
Managing contagion in the family
Ringworm is less contagious just a few days after starting the correct therapy, but it is important to take some precautions to prevent it from spreading to other family members or from affecting the child again. Here are the main measures:
- wash towels, sheets and clothing at 60°C or higher;
- do not share combs, brushes, hats or pillows until you heal;
- disinfect frequently used surfaces and objects, such as remote controls, games, chairs or carpets;
- if you have pets, have the skin checked by the vet, because they can harbor zoophilic fungi;
- Avoid direct skin-to-skin contact in infected areas until your doctor confirms there is no longer a risk.
Following these simple rules helps eliminate fungal spores from the environment and prevents relapses.
Possible complications of ringworm
In most cases, ringworm is a benign infection and heals without leaving any signs. However, if untreated or very inflammatory, it can cause some complications:
- Bacterial superinfection. Scratches and irritated lesions can become infected with skin bacteria, such as staphylococci or streptococci.
- Permanent hair loss. Some forms of tinea capitis, especially those with kerions, can leave small areas of cicatricial alopecia if not treated promptly.
- Persistent nail changes. In tinea unguium, the nail may remain thickened or brittle even after healing.
- Serious infections in the immunocompromised. In children with very low immune defenses, dermatophytes can cause more extensive and difficult to treat forms.
These complications are rare, but highlight the importance of early diagnosis and immediate initiation of therapy.
How to prevent ringworm: practical advice
Ringworm can be prevented with a little daily attention. It is important to keep your skin dry, especially after sport or shower, and use breathable clothing that reduces sweat and irritation.
Children should not share combs, brushes, hats or towels, especially in the event of outbreaks at school. In public environments such as swimming pools or changing rooms it is best to avoid walking barefoot.
Pets can also be a source of contagion: if they have hairless areas or scabs, it is best to have them checked by the vet. If there is a case of ringworm in the family, just follow the indicated therapy and limit skin-to-skin contact on the infected area for a few days to reduce the risk of transmission.
Conclusions
Ringworm is an annoying infection but in the vast majority of cases easy to recognize and treat. With a timely diagnosis, adequate therapy and some targeted hygiene measures, children recover completely and without consequences. Knowing how it manifests itself and how it can be prevented helps families manage it with peace of mind.